
As of February 1, 2016 the Shared Responsibility Employer Mandate aspect of the Patient Protection and Affordable Care Act (ACA) reporting requirements became effective for all employers.
The mandate involves a multi-step process for employers and a filing with the Internal Revenue Service (IRS), which went into effect at the beginning of this year. This will also require an additional figure entered into employee W-2 forms showing the total value of coverage during the calendar year.
ACA Reporting Requirements and ALEs
Companies with 50 or more full-time employees throughout a calendar year are considered to be an applicable large employer, ALE, and must fulfill the employer mandate. Consequently, for ALE employers, the distinction between full and part-time employees is a significant issue.
In fact, many larger retail businesses with predominately part-time employees are having to make major adjustments. It has been common to use 35 hours worked weekly as the definition of a part-time staffer for the companies. Now this will have to be scaled back in order to avoid costly health coverage requirements.
There are two methods for defining full-time workers, according to the IRS:
“For purposes of the employer shared responsibility provisions, a full-time employee is, for a calendar month, an employee employed on average at least 30 hours of service per week, or 130 hours of service per month.
There are two methods for determining full-time employee status:
- The monthly measurement method, and
- The look-back measurement method.
Under the monthly measurement method, the employer determines if an employee is a full-time employee on a month-by-month basis by looking at whether the employee has at least 130 hours of service for each month.
Under the look-back measurement method, an employer may determine the status of an employee as a full-time employee during what is referred to as the stability period, based upon the hours of service of the employee in the preceding period, which is referred to as the measurement period. The look-back measurement method may not be used to determine full-time employee status for purposes of ALE status determination.”
ACA Reporting Requirements Now Include Smaller Employers
Companies with 100 or more full-time employees were required to file proof of healthcare coverage for the 2014 tax year. The government delayed the employer mandate for businesses with 50-99 employees until this year.
More specifically, for the 2015 tax year, larger employers are required to offer coverage to 95% of full-time staff, and companies in the smaller category must meet a 70% threshold, which is set to increase to 95% this year.
The IRS stipulates safe harbors to help companies determine if their employer-sponsored health insurance plans qualify for the ACA’s affordability standard. According to the IRS, health insurance costs must now be less than 9.66% of the individual’s annual household income as of 2016, up from the previous level of 9.5%.
According to the IRS Website,
“an employer may choose to use one or more of the safe harbors for all of its employees or for any reasonable category of employees, provided it does so on a uniform and consistent basis for all employees in a category. If an employer offers multiple healthcare coverage options, the affordability test applies to the lowest-cost self-only option available to the employee that also meets the minimum value requirement.”
Reporting Requirements and Forms
Companies must complete IRS Form 1094-B, Transmittal of Health Coverage Information Returns, and Form 1095-B, Health Coverage. Form 1095-B contains the requisite information, including the filer’s identifying data, names of insurance issuers and a listing of individuals covered.
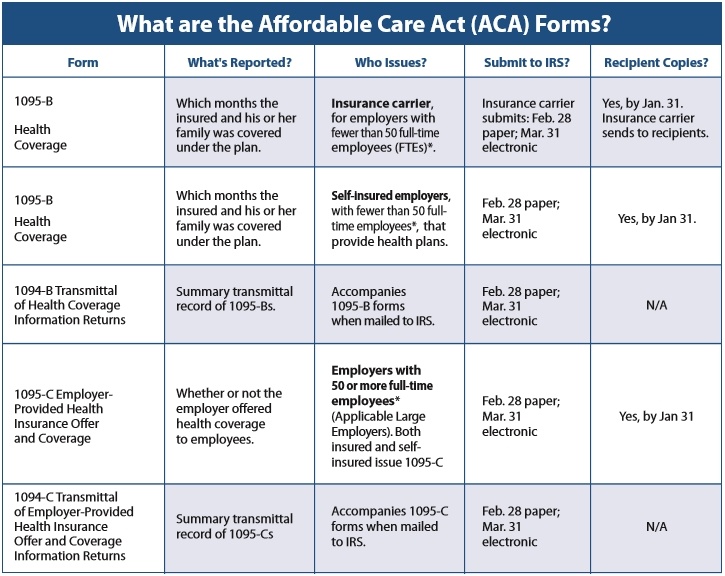
Any business submitting 250 or more returns is required to file electronically.
Additionally, as of February 1, 2016, the law requires businesses to supply employees with a hard copy of this information. Employees can give employers permission to provide the forms electronically.
Noncompliance can result in penalties of $100 for each return failure, not to exceed $1.5 million per year. Fines are also applied for failure to disseminate individual payee statements.
Employers and HR Professionals Have Help for Navigating the ACA Requirements
An updated and streamlined reporting strategy will help your organization meet its obligations, while providing accuracy and timeliness. So take time to understand the law and prioritize accurate record keeping. In this way, you will make compliance a sure thing.
Another key step in maintaining HR compliance and increasing your company's cost-effectiveness is to consider outsourcing. A professional agency such a Accuchex can provide much-needed help with Human Resources needs and questions. Accuchex is a full spectrum Payroll Management Services provider offering expertise in Time Management, Insurance and Retirement issues, as well.


